Your dog's diet is a powerful tool to effectively manage various medical conditions
Diet for dogs with liver disease
If your dog has been diagnosed with liver disease and you would like help creating a safe, balanced home-prepared diet, you can learn more about my nutrition consultations below.
Updated March 2026 by Kristina Johansen
What can I feed my dog with liver disease?
The liver is a very complicated and hard-working organ. It’s also unique in that it can repair and regenerate itself – as long as enough healthy tissue remains and it’s given the right support.
The liver works hand in hand with the digestive system. Almost everything your dog eats or drinks eventually passes through the liver, where it’s processed, filtered, and transformed.
Because of this, the liver is especially vulnerable to anything that enters through food, water, or medication. When the liver is damaged, it can no longer do its many jobs efficiently. That’s why nutritional support is key for dogs with liver disease or damage.
In this guide, our focus is on the dietary management of three common liver conditions.
- Part 1: Acute or chronic hepatitis – inflammation and scarring of the liver
- Part 2: Portosystemic shunt – often called a liver shunt
- Part 3: Copper-associated hepatopathy – also known as copper storage disease
Each of these conditions affects the liver in its own way. Rather than grouping them together, I’ve separated them into three parts to help you better understand the mechanisms without oversimplifying or overwhelming you.
This is a long guide, so feel free to jump straight to the section that applies to your dog by clicking the headings above. However, there’s some overlap between the conditions, so you may still find it helpful to skim the other parts too.
Let’s dive in!
Part 1: Dietary management of chronic hepatitis in dogs (inflammation of the liver)
Chronic hepatitis (CH) means long-term inflammation within the liver. It isn’t one single disease, but rather a condition that can develop for many different reasons. Regardless of the cause, the underlying issue is the same: the liver becomes damaged and, over time, can begin to lose some of its ability to function.
Because the liver plays such a central role in metabolism, digestion, and detoxification, nutrition becomes a vital part of supporting dogs with chronic hepatitis. The aim isn’t just to “rest” the liver; it’s to reduce ongoing inflammation, support regeneration of liver cells, and make sure your dog is getting everything they need without creating extra stress for the liver.
Understanding what the liver is struggling with
In healthy dogs, the liver filters toxins, processes nutrients, makes proteins and helps regulate fat, carbohydrate, and vitamin metabolism. In chronic hepatitis, inflammation disrupts these processes. Over time, scar tissue can build up (fibrosis), progressively limiting what the liver can do.
This means a few things become especially important when designing a diet:
- Protein must be adequate but not excessive
- Fat intake may need adjusting, particularly when bile flow or fat digestion is affected
- Antioxidants and certain nutrients can help protect liver cells.
Protein
Unlike dogs with portosystemic shunts, most dogs with chronic hepatitis do not require dietary protein restriction, provided there are no signs of hepatic encephalopathy (HE) – you can read more about HE in the second part of this post. Instead, the aim is to feed an appropriate amount of well-tolerated protein to maintain lean body mass and help prevent cachexia (the loss of muscle mass), without overloading the liver.
To do this, it’s important to focus on protein quality rather than quantity. High-quality protein is easy to digest and efficiently used by the body. It provides the amino acids needed to maintain muscle mass and support healing, while producing fewer waste products (such as nitrogen compounds) for the liver to clear.
Examples of high-quality, well-tolerated protein sources include egg, poultry, white fish, tofu and dairy.
Fat
Fat increases calorie density and palatability, which is especially important for dogs that may not eat much and need support in maintaining body condition. Fat also supplies essential fatty acids and helps the body absorb fat-soluble vitamins (A, D, E and K). For this reason, fat does not usually need to be restricted in dogs with chronic hepatitis.
One important exception is dogs with blocked or damaged bile ducts, where bile cannot flow properly from the liver into the gut. Bile is essential for digesting fat, so when too little bile reaches the intestines, fat becomes difficult to break down and absorb. This can lead to signs such as very pale stools, yellowing of the skin or eyes (jaundice), easy bruising or bleeding, and digestive upset. In these cases, higher-fat diets can worsen symptoms because the body simply can’t handle fat efficiently.
Carbohydrates and fibre
Carbohydrates (glucose) are your dog’s main source of energy. In healthy dogs (and people), the liver acts as the body’s main “glucose manager”. It produces and releases most of the glucose (sugar) needed to keep vital cells alive, including the brain and red blood cells.
It is therefore not surprising that when the liver is damaged, glucose storage and production can be affected. Most dogs with chronic liver disease maintain normal blood sugar levels. However, in sudden and severe liver failure, or in very young dogs with liver problems, the liver may struggle to regulate glucose, and some dogs can develop low blood sugar (hypoglycaemia)
For this reason, the amount and type of carbohydrate should be tailored to how well your dog can maintain normal blood sugar levels. Dogs that are “metabolically stable” can keep both blood sugar and energy levels within a healthy range.
In contrast, a ‘metabolically unstable’ dog might develop low blood sugar, lose weight, or show signs of hepatic encephalopathy (HE).
That’s why carbohydrate type and amount should be chosen based on how stable (or unstable) a dog’s metabolism is, especially the ability to maintain normal blood glucose.
Highly digestible carbohydrates such as well-cooked white rice, pasta, or peeled potatoes are especially useful for hypoglycaemic dogs (dogs with low blood sugar) or dogs that are short on energy. Soluble fibres (such as psyllium husk) can support ammonia control in dogs showing signs of hepatic encephalopathy.
In practice, this means there is no single “ideal” carbohydrate source or amount; choices should be guided by the individual dog.
Antioxidants
Long-term inflammation produces oxidative stress, which damages liver cells and contributes to the progression of fibrosis (scarring). Antioxidant support should therefore be part of dietary management as it may help protect liver cells and support regeneration.
Commonly used antioxidants include:
- Vitamin E – supports cell membrane health and reduces oxidative damage.
- SAMe – boosts glutathione production, one of the liver’s most important natural antioxidants.
- Silymarin/milk thistle – may help protect liver cells and support regeneration.
- Omega-3 fatty acids (from fish oil) – may help modulate inflammation.
Copper
Not all cases of chronic hepatitis involve copper, but copper accumulation is common enough that it’s worth mentioning. If blood tests or a liver biopsy show elevated copper levels, dietary copper restriction becomes crucial. If copper levels are normal, copper restriction isn’t usually necessary. You can read more in Part 3: Dietary management of copper-associated hepatopathy (copper storage disease) in dogs.
Appetite support
Many dogs with chronic hepatitis experience nausea or poor appetite. Offering multiple small meals, warming food slightly, adding moisture, or rotating between acceptable protein sources can make eating easier.
What this means in practice
- Feed high-quality, highly digestible proteins such as eggs, poultry, fish, tofu, or dairy.
- Protein doesn’t usually need to be heavily restricted unless hepatic encephalopathy develops.
- Adjust dietary fat based on individual tolerance.
- Carbohydrate amount and type should be chosen based on your dog’s metabolic stability and clinical status.
- Include antioxidants such as vitamin E, SAMe, silymarin, and omega-3 fatty acids.
- Restrict copper only if your dog has evidence of, or is suspected of, copper accumulation.
- Offer smaller, more frequent meals to reduce nausea and improve appetite.
- Always ensure access to fresh water and monitor weight and muscle condition regularly.
Part 2: Dietary management of portosystemic shunt (liver shunt) in dogs
To better understand why certain dietary changes are needed, it helps to first look at what happens inside your dog’s body when a liver shunt is present.
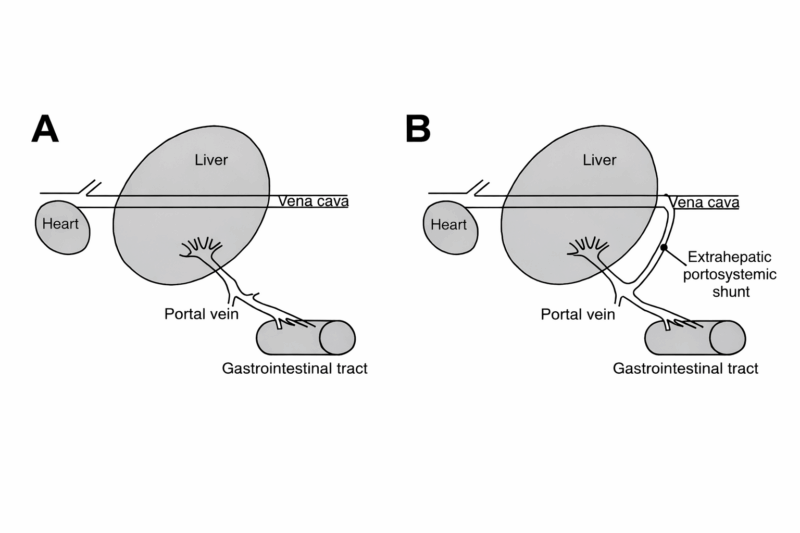
A liver shunt is a fault in your dog’s blood vessels. Instead of blood passing through the liver to be cleaned and processed, it diverts around it. This means toxins, nutrients, and other substances that should be filtered by the liver end up circulating in the body instead.
Here is a simplified drawing illustrating a normal liver (A) versus a liver shunt (B). You can see how the blood bypass the liver and enters circulation.
Hepatic encephalopathy (HE)
When a dog is diagnosed with a liver shunt (also called a portosystemic shunt, or PSS), one of the biggest concerns is how this condition affects the brain. The medical term for this is hepatic encephalopathy (HE).
HE happens when substances that would normally be processed by the liver build up in the bloodstream, causing a range of problems, from mild confusion or odd behaviour after meals, to seizures or, in severe cases, coma.
One of the main substances involved is ammonia. Ammonia is produced when your dog digests protein. In a healthy dog, the liver converts ammonia into a safer waste product called urea. Urea is then carried to the kidneys and excreted in the urine.
In dogs with a liver shunt, blood bypasses the liver. This means ammonia is not properly converted into urea and instead circulates in the bloodstream. As levels rise, ammonia can affect the brain and trigger signs of HE.
Because ammonia is a by-product of protein metabolism, protein intake becomes a key consideration when managing dogs with liver shunts.
The protein puzzle
It might seem logical to assume that simply restricting protein will solve the ammonia problem. While reducing protein can lower ammonia production, the situation is more nuanced. Striking the right balance is crucial. Too little protein can lead to muscle wasting, while too much, or the wrong type, can worsen HE.
As a rule of thumb:
- If a dog has a liver shunt but no signs of HE, protein doesn’t usually need to be severely restricted. These dogs can often eat moderate levels of ‘HE-friendly’ proteins.
- If a dog shows signs of HE, both the type and the amount of protein become equally important.
So, what are ‘HE-friendly’ proteins?
HE-friendly proteins are those that are highly digestible and therefore tend to result in less ammonia production in the colon. These include dairy proteins, such as yoghurt and cottage cheese; eggs; and vegetable proteins, such as soy (tofu). Diets based on these protein sources are often better tolerated in dogs with hepatic encephalopathy.
White fish such as cod, haddock and pollock also produce relatively little ammonia. However, they are high in purines, which can increase the risk of urate bladder stones in dogs with liver disease.
Let’s take a closer look at why that happens.
Liver shunts, purines and urate stones
Purines are natural compounds found in many foods, such as organ meats, certain seafoods and most meats. When your dog digests these foods, the purines are broken down into uric acid. In healthy dogs, the liver then converts uric acid into a harmless, water-soluble substance called allantoin, which is excreted in the urine.
In dogs with a liver shunt, blood bypasses the liver, so this conversion doesn’t happen properly. As a result, uric acid builds up in the body and spills into the urine. When uric acid and ammonium meet in the bladder or kidneys, they can combine to form ammonium urate crystals and stones.
For this reason, foods high in purines are also best avoided in dogs with shunts. The good news is that the same protein sources that produce less ammonia, such as eggs, dairy and soy, are also naturally low in purines. Choosing these proteins helps reduce the risk of hepatic encephalopathy and urate stones at the same time.
Dietary fibre
Dietary fibre, such as psyllium husk, can be very helpful for dogs with liver disease, particularly when hepatic encephalopathy is a concern. Why? Because fibre changes what happens inside the gut in a way that helps reduce how much ammonia enters the bloodstream.
When fermentable fibre reaches the large intestine, friendly gut bacteria break it down and produce natural acids. These acids make the gut slightly more acidic, which turns ammonia into a form that is much harder for the body to absorb. This helps keep more ammonia inside the gut, so it can be passed out in the stools instead of reaching the brain.
Fibre also feeds beneficial gut bacteria and shifts the balance away from bacteria that produce large amounts of ammonia from protein. In short, it supports a healthier gut environment that produces fewer toxins in the first place.
Dogs vary widely in how they respond to both the amount and type of dietary fibre. Some will show improved stool quality and gastrointestinal comfort, while others may develop constipation, diarrhoea, or increased flatulence. For this reason, fibre should be introduced gradually, and the dog’s individual response monitored closely, whether fibre is increased through diet composition or added as a supplement.
What this means in practice
- Dogs with a liver shunt should avoid meat-based protein, especially organ meats.
- Prioritise egg, dairy, and soy protein to help manage both hepatic encephalopathy (HE) and urate stone formation.
- Protein doesn’t usually need to be drastically reduced, but it should be carefully managed. The trick is feeding the type and amount your dog can tolerate without developing HE.
- Offer small, frequent meals to help reduce post-meal ammonia spikes and minimise the risk of HE signs.
- Include dietary fibre to support gut health and help lower ammonia absorption.
- Always ensure your dog has constant access to fresh water.
Part 3: Dietary management of copper-associated hepatopathy (copper storage disease) in dogs
Copper is a trace mineral essential to health. It helps your dog’s body make energy, build strong tissues, and protect cells from damage. It is absorbed in the small intestine, carried through the blood, and stored safely in the liver until needed. Any extra is simply passed out in the stool.
The problem arises when copper isn’t properly processed and starts to build up in the liver. Over time, this buildup becomes toxic and begins to damage liver cells. This condition is called copper storage disease, or copper-associated hepatopathy.
Why did copper build up in my dog’s liver?
There are two main reasons why dogs may accumulate copper in the liver. It can happen due to either one of these reasons, or sometimes a combination of both.
1. Genetic susceptibility
Some dogs are born with a higher risk of copper build-up because of the way their genes control copper handling. In Bedlington Terriers, this was once thought to be due to a single faulty gene called COMMD1. We now know the story is more complex. Several genes, including ATP7B, can also play a role. This means copper toxicosis in Bedlington Terriers isn’t always explained by just one mutation alone.
Other breeds – such as Labradors, Dobermans, Dalmatians, and West Highland White Terriers – also carry genetic variants that make them more vulnerable. For example, in Labradors, researchers have found changes in the ATP7B and ATP7A copper transport genes that affect how efficiently copper is processed.
It is important to note that these genetic variants don’t automatically cause disease; instead, they increase the risk. Copper storage disease in dogs is complex and influenced by multiple factors, including diet, environment and other genes.
2. Dietary intake
Over the past few decades, several studies have found that copper levels in dogs’ livers are creeping up. So why is this happening? Research suggests that modern commercial dog foods may be part of the reason, possibly due to changes in the types of copper used in dog food.
Why is excess copper a problem?
Excess copper in the liver can trigger harmful chemical reactions. Think of it like a loose spark in a dry forest – it sets off damaging chain reactions. It reacts with unstable molecules (free radicals) to create even more highly reactive particles known as hydroxyl radicals. These attack cell membranes, proteins, and even DNA.
Over time, this ongoing damage causes oxidative stress, which leads to liver inflammation and, eventually, long-term inflammation and scarring of the liver – a condition known as chronic hepatitis.
That’s why providing the right nutrition alongside antioxidant support is a key part of treatment. It helps protect the liver and slow further damage.
Copper restriction
Given that copper accumulation is central to the problem, it’s no surprise that copper restriction is one of the most important steps we can take to manage the disease. Of course, restriction is a relative term. I generally aim to keep copper intake close to the NRC minimum requirement.
- Foods high in copper include liver, kidney, shellfish, nuts, mushrooms, lentils, lamb, and duck.
- Foods lower in copper include white rice, yoghurt, eggs, chicken breast, cod, cottage cheese, and pasta.
The role of zinc
Zinc competes with copper for absorption in the intestine. It also triggers the body to produce a protein called metallothionein, which binds to copper and prevents it from entering the bloodstream. As the intestinal cells naturally shed, the bound copper is carried out of the body in the stool.
For this reason, I often see dog owners adding zinc supplements to their dog’s diet when their dog is diagnosed with liver disease. This is risky without a vet or nutritionist to monitor your dog, and should not be done on your own.
Yes, zinc can be helpful for dogs with copper-related liver disease, but the timing matters. In many cases, vets first use special medicines called chelators to remove excess copper that’s already stored in the liver. Zinc usually isn’t started at the same time as these drugs.
The reason is simple: chelators don’t just bind copper – they also grab onto zinc. If zinc is given at the same time, the two can effectively cancel each other out, making both treatments less effective.
Once chelation has done its job and liver copper levels have come down, zinc is often added to the plan. At this stage, zinc helps by reducing how much copper is absorbed from the gut, which can slow or prevent copper from building up again.
Zinc still needs to be used carefully and under veterinary supervision. Too much can upset the stomach and can also interfere with the body’s balance of copper and iron. This is why blood tests – and sometimes liver tests – are used to make sure zinc is helping rather than causing new problems.
Protein
Dogs with copper storage disease still need enough protein to maintain muscle and help the liver repair itself. In most cases, protein does not need to be heavily restricted (unless a portosystemic shunt is present). The focus is instead on providing high-quality, easily digestible proteins such as eggs, poultry, white fish, or dairy.
Antioxidant support
Because copper toxicity drives oxidative stress, antioxidants play a vital role in protecting the liver. They help by neutralising damaging free radicals and giving liver cells a chance to repair.
Commonly used options include:
- Vitamin E – Protects liver cell membranes from oxidative damage.
- SAMe (S-adenosylmethionine) – A building block for glutathione, the liver’s main antioxidant.
- Milk thistle (silymarin, silybin) – A herbal extract with both antioxidant and liver protective properties.
These supplements are not a replacement for copper control, but they can provide valuable extra support for liver health.
What this means in practice
- Keep copper intake close to the NRC minimum requirement
- Avoid high-copper foods such as liver, kidney, nuts, mushrooms, lentils, lamb, and duck.
- Prioritise high-quality, easily digestible protein from eggs, poultry, white fish, or dairy.
- Antioxidants such as vitamin E, SAMe, and milk thistle can help protect the liver from further oxidative damage.
About Kristina
Kristina Johansen, MSc cand. (Animal Nutrition), Cert ACN, is a dog nutritionist with over 15 years of experience. She is a member of the American Academy of Veterinary Nutrition (AAVN) and the European Society of Veterinary & Comparative Nutrition (ESVCN). She specialises in formulating balanced home-prepared diets that meet NRC guidelines, particularly for dogs with medical conditions that require careful dietary management. Learn more →Disclaimer: The information provided in this blog is meant for informational and educational purposes only. Please don’t try to create or modify your dog’s diet based on the information provided. Diet formulation for dogs with health concerns is complex. If you’re considering a homemade diet for your dog, please ensure it is formulated by a qualified dog nutritionist.
Dog Nutrition Consultations
If your dog has been diagnosed with liver disease and you would like help creating a safe, balanced home-prepared diet, you can learn more about my nutrition consultations below.
Book a Consultation